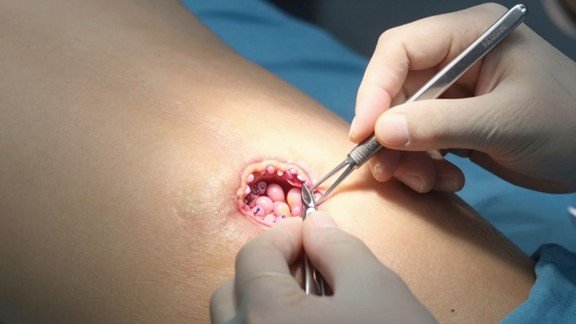
What Constitutes Abdominal Wall Reconstruction?
Abdominal wall reconstruction is a surgical process. It’s used to fix a weakened or damaged abdominal wall. This often happens because of a hernia. Think of it as rebuilding the core structure of your abdomen. It’s not just a simple patch-up job. Instead, it involves complex techniques to restore both form and function. This type of surgery is typically reserved for larger, more complicated hernias, or those that have come back after previous repairs. It’s a significant procedure aimed at long-term success.
The Complex Anatomy of the Abdominal Wall
The abdominal wall is surprisingly intricate. It’s not just a single layer of muscle. Several layers of muscles and connective tissues work together. These include the rectus abdominis, external obliques, internal obliques, and the transversus abdominis. Each plays a role in supporting your organs and allowing for movement. Understanding this complex anatomy is key to successful abdominal wall reconstruction. When this structure is compromised by a hernia, it affects more than just appearance; it impacts core strength and stability.
When Is Reconstruction Necessary?
Reconstruction becomes necessary when a hernia is too large or complex for simpler repair methods. It’s also indicated for recurrent hernias, meaning they’ve reappeared after a prior surgery. Sometimes, trauma or previous surgeries can weaken the abdominal wall significantly. In these cases, a standard repair might not hold. Abdominal wall reconstruction offers a more robust solution. It addresses the underlying weakness and aims to prevent future problems. It’s a solution for when the abdominal wall needs more than just a basic fix.
Candidates for Hernia Surgery
Identifying Patients Who Need Reconstruction
Not everyone with a bulge needs surgery right away, but some hernias definitely do. If you have a hernia that causes pain, makes it hard to do daily tasks, or just won’t go back in on its own, it’s time to talk to a doctor. This is especially true for hernias that have been there a while or are quite large. These kinds of hernias often won’t fix themselves and can lead to bigger problems down the road if left untreated. The goal is to get you back to normal life without the worry of a hernia.
Sometimes, a hernia might pop up after surgery, known as an incisional hernia. You might see a bulge near an old scar. Discomfort when bending or lifting is common. These often require surgical attention. The decision for hernia surgery is based on symptoms and the hernia’s characteristics. It’s not just about the bulge; it’s about how it affects your life and health.
The Importance of Pre-Operative Management
Getting ready for hernia surgery is more than just picking a date. Doctors will look at your whole health picture. This includes checking your medical history and any other health issues you might have. They’ll also review your medications, including any supplements or herbs you take. This step is vital to make sure you’re in the best shape possible for the procedure.
Sometimes, you might need extra tests like blood work or imaging. If you smoke, quitting before surgery can make a big difference in healing. Managing conditions like diabetes is also key. The aim is to reduce any risks associated with the surgery and help your recovery go smoothly. This preparation is a big part of successful hernia surgery.
Personalized Surgical Planning
Once you’re cleared for surgery, the plan becomes very specific to you. Your surgeon will discuss the best approach, whether it’s open, laparoscopic, or robotic. This choice depends on the type and size of your hernia, as well as your overall health. They’ll explain what to expect during the procedure and what kind of anesthesia you’ll have.
It’s important to ask questions. Understanding the steps involved helps ease anxiety. You’ll get instructions on what to do before surgery, like when to stop eating or drinking. Arranging a ride home afterward is also a must, as you won’t be able to drive yourself. This detailed planning ensures the best possible outcome for your hernia repair.
The decision for hernia surgery is a collaborative one between patient and surgeon, focusing on symptom relief and long-term health.
| Factor | Consideration | |
| Hernia Size & Location | Affects surgical approach and complexity | |
| Patient Symptoms | Pain, discomfort, impact on daily activities | |
| Previous Surgeries | May complicate the repair | |
| Overall Health Status | Comorbidities, age, and physical condition |
Surgical Techniques in Hernia Repair
Open Surgical Approaches
Open surgery is a traditional method for hernia repair. It involves a larger incision directly over the hernia. This approach allows the surgeon direct access to the hernia site. It’s often chosen for very large or complex hernias, or when there’s a need to remove excess tissue. The surgeon can clearly see and work with the abdominal wall structures. This method is straightforward and has been used for many years.
Minimally Invasive Laparoscopic Methods
Laparoscopic surgery, often called “keyhole surgery,” uses small incisions. A thin tube with a camera, called a laparoscope, is inserted through one small cut. This camera projects images onto a screen, guiding the surgeon. Surgical instruments are then inserted through other small incisions to perform the repair. This technique generally leads to less pain and a quicker recovery compared to open surgery. It’s a popular choice for many types of hernias.
Robotic-Assisted Hernia Surgery
Robotic-assisted surgery is a type of minimally invasive procedure. The surgeon operates from a console, controlling robotic arms that hold specialized surgical instruments. This technology offers enhanced precision and dexterity. The surgeon’s view is often magnified, providing a detailed look at the surgical field. This method can be beneficial for complex repairs, allowing for meticulous work through small incisions. The goal is to achieve a strong repair with minimal disruption.
Specific Hernia Repair Procedures
Retro-Rectus Rives Stoppa Repair
This method focuses on strengthening the abdominal wall from behind the rectus abdominis muscles. Surgeons carefully dissect the space behind these muscles, creating a larger area to place a mesh prosthesis. This technique aims to reduce tension on the repair site. The Rives Stoppa repair is often chosen for larger hernias.
Anterior Component Separation Techniques
Anterior component separation involves making a controlled incision in the external oblique muscle. This allows the surgeon to bring the rectus abdominis muscles closer together without excessive pulling. This approach is useful when the abdominal wall is too tight for a direct repair. Mesh is typically placed between the skin and the abdominal muscles in this procedure.
Posterior Component Separation (Transversus Abdominis Release)
Posterior component separation, also known as Transversus Abdominis Release (TAR), is a more extensive technique. It involves releasing the transversus abdominis muscle, the deepest abdominal muscle. This provides significant room to close large abdominal wall defects. TAR is often reserved for very complex or recurrent hernias. The goal of these specific hernia repair procedures is to achieve a tension-free closure and a durable repair.
The Role of Surgical Mesh
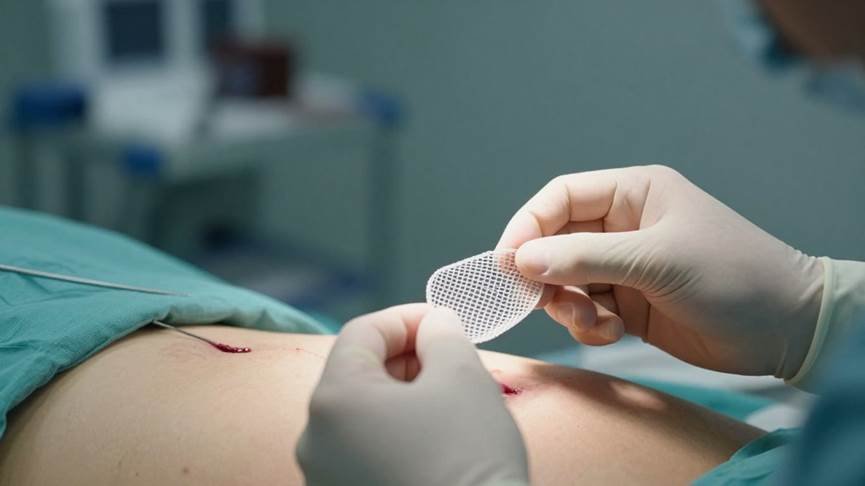
Mesh as Reinforcement in Hernia Surgery
When surgeons repair abdominal wall hernias, they often use surgical mesh. Think of it like patching a hole in a wall. This mesh acts as a strong support system. It helps reinforce the weakened area of the abdominal wall. This is especially important for larger hernias or when the tissue is very thin. The goal is to give the body a solid foundation to heal around.
Understanding Mesh Placement
Where the mesh goes matters a lot. Surgeons can place it in different spots relative to the abdominal muscles. Sometimes it’s put in front of the muscles, and other times it’s placed behind them. The specific placement depends on the type of hernia and the surgical technique used. The aim is always to secure the mesh properly so it can do its job effectively. Proper placement is key to a successful repair.
Long-Term Benefits of Mesh Use
Using surgical mesh significantly lowers the chances of a hernia coming back. It helps the body build new tissue around it, creating a stronger, more stable abdominal wall. This means fewer worries about future problems. While there are always risks with any surgery, the benefits of mesh in preventing hernia recurrence are well-established. It’s a common tool that helps patients get back to their normal lives with more confidence.
Preparing for Hernia Surgery
Medical History Review and Assessments
Before any hernia surgery, a thorough review of your medical history is a must. This isn’t just a formality; it’s about safety. Doctors need to know about any past surgeries, existing conditions like heart problems or diabetes, and any previous issues with anesthesia. They’ll also ask about allergies, especially to latex or certain medications. This information helps the surgical team plan the best approach for your specific situation and minimize risks. It’s important to be completely open and honest during this assessment.
Medication Adjustments Before Surgery
Certain medications can affect your surgery and recovery. Blood thinners, for example, might need to be stopped or adjusted days or even weeks before your procedure to reduce bleeding risks. Even over-the-counter drugs, vitamins, and herbal supplements can interact with anesthesia or affect healing. Your doctor will provide clear instructions on which medications to continue, stop, or change. Following these medication adjustments precisely is vital for a smooth surgical experience and successful hernia repair.
Pre-Operative Instructions and Fasting
As your surgery date approaches, you’ll receive specific instructions. These often include guidelines on when to stop eating and drinking. This fasting period is critical for anesthesia safety, preventing complications like aspiration. You’ll also be told when to arrive at the hospital and what to bring. Don’t hesitate to ask questions about anything unclear. Proper preparation is key to a successful hernia surgery.
Following all pre-operative instructions, including dietary restrictions and medication changes, is paramount. This preparation directly impacts the safety and effectiveness of the hernia repair procedure.
The Hernia Surgery Procedure
Anesthesia Options for Hernia Repair
When it comes to hernia surgery, anesthesia is a big part of the process. The type of anesthesia used really depends on the specific hernia repair procedure and what the surgeon thinks is best for the patient. For many open surgeries, a local anesthetic might be enough, meaning you’re awake but the area is numb. Sometimes, a regional anesthetic is used, which numbs a larger area. For laparoscopic or robotic procedures, general anesthesia is more common. This puts you completely to sleep for the duration of the hernia surgery.
The goal is always to keep you comfortable and pain-free throughout the entire operation. Your surgical team will discuss these options with you beforehand to make sure you understand what to expect. They’ll consider your overall health and any specific needs you might have when making the final decision about the anesthesia for your hernia repair.
Tissue Repair and Reinforcement
Once you’re prepped and comfortable, the actual repair work begins. The surgeon’s main job is to put any bulging tissue back where it belongs and then fix the weakened spot in the abdominal wall. This often involves stitching healthy tissue together to create a stronger barrier. For many hernia repair procedures, especially those involving larger defects or a higher risk of recurrence, surgical mesh is used.
This mesh acts like a patch, providing extra support to the weakened area. It’s typically made of a material that the body can integrate with over time, becoming a permanent part of the abdominal wall. The placement and type of mesh are carefully chosen based on the hernia’s location and size, as well as the surgical approach taken. Using mesh is a common practice in hernia surgery to improve the long-term success rate.
Duration of Hernia Surgery
The time it takes for hernia surgery can really vary. Simple repairs, especially those done laparoscopically, might only take about 30 minutes to an hour. However, more complex cases, like those involving large hernias, multiple hernias, or extensive tissue repair, can take significantly longer. Sometimes, a complex open hernia surgery could last up to five hours.
Factors influencing the duration include the size and location of the hernia, whether mesh is being used, and the surgeon’s experience. Robotic-assisted procedures can sometimes take a bit longer than traditional laparoscopic surgery due to the setup time involved. Your surgical team will give you an estimate beforehand, but it’s important to remember that patient safety is always the top priority, and the procedure will take as long as needed to be done correctly.
The success of hernia surgery relies on precise tissue handling and appropriate reinforcement, whether through natural tissue repair or the use of surgical mesh. The duration is secondary to achieving a durable and effective repair.
Post-Operative Recovery and Outlook
Immediate Post-Surgery Monitoring
After hernia surgery, patients are closely watched. This happens first in a recovery room. Nurses check vital signs and how well the patient is tolerating pain medication. They also monitor for any immediate issues. The goal is to ensure a stable transition from anesthesia. Patients might stay in the hospital for a few days, depending on the surgery’s complexity. This period is key for managing initial pain and checking the surgical site.
Activity Restrictions and Gradual Return
Movement is important after surgery, but it needs to be managed. Patients are encouraged to walk short distances soon after the procedure. This helps prevent blood clots and aids in recovery. Heavy lifting and strenuous activities are off-limits for several weeks. A gradual return to normal activities is advised. This means slowly increasing physical exertion over time. Listen to your body; rest when needed. Walking is a great way to start regaining strength.
Potential Complications and Management
While hernia surgery is generally safe, complications can occur. These might include infection, bleeding, or issues with wound healing. Blood clots are also a risk. Patients are given medication to help prevent them. Chronic pain is another possibility, though less common. It’s important to know the signs of trouble. Contacting the medical team promptly is vital if any concerns arise. Early detection and management are key to a good outcome after hernia surgery.
Key Recovery Points:
- Pain Management: Medications will be prescribed. Take them as directed.
- Wound Care: Keep the incision clean and dry. Follow specific instructions.
- Hydration & Diet: Drink plenty of fluids and gradually return to a normal diet.
- Follow-Up: Attend all scheduled appointments with your surgeon.
Recovery timelines vary. Some patients feel significantly better within a few weeks, while others may take a couple of months to feel fully back to normal. Patience and adherence to medical advice are crucial.
Wrapping Up Hernia Surgery
So, when it comes to those tricky abdominal wall hernias, surgery really is the main way to fix them for good. Whether it’s a simple repair or a more involved reconstruction, the goal is to get things back where they belong and stop that bulge from causing trouble. While recovery takes a bit of time and patience, most people find that getting back to normal life without the discomfort is totally worth it. It’s all about getting your core strength back and feeling more comfortable in your own skin.